Dental Care for Diabetic Patients in Scottsdale, AZ
 If you have diabetes, the standard recall schedule isn’t always the right fit, and at GOREgeous Smiles in Scottsdale, AZ, we adjust your visits to match how diabetes actually affects your mouth. Chronically elevated blood sugar feeds inflammation in gum tissues and slows the body’s response to bacterial infection, which is why gum disease tends to be more common, more aggressive, and harder to control in patients with diabetes than in the general population. If you have diabetes, the standard recall schedule isn’t always the right fit, and at GOREgeous Smiles in Scottsdale, AZ, we adjust your visits to match how diabetes actually affects your mouth. Chronically elevated blood sugar feeds inflammation in gum tissues and slows the body’s response to bacterial infection, which is why gum disease tends to be more common, more aggressive, and harder to control in patients with diabetes than in the general population.
What we want every diabetic patient to know is that this isn’t a one-way street. Active gum disease can make blood sugar harder to control, so the dental side of your care isn’t separate from your diabetes management – it’s part of it. We coordinate with your primary care provider or endocrinologist when that helps, and we adapt your visits in concrete ways that match your situation.
Dental care for diabetic patients fits inside our broader preventive dentistry, but it deserves its own focused conversation. The stakes and the schedule both look different, and the choices we make together – how often you come in, what we screen for, how we time procedures – depend on what’s happening with your blood sugar control.
On This Page
What Is Dental Care for Diabetic Patients?
 Dental care for diabetic patients is the same dentistry – cleanings, exams, fillings, restorations – adjusted for how diabetes changes the mouth. The differences aren’t dramatic on most days, but they add up over time, and small adjustments now prevent a lot of problems we’d otherwise have to treat later. Dental care for diabetic patients is the same dentistry – cleanings, exams, fillings, restorations – adjusted for how diabetes changes the mouth. The differences aren’t dramatic on most days, but they add up over time, and small adjustments now prevent a lot of problems we’d otherwise have to treat later.
Why Diabetes and Oral Health Affect Each Other
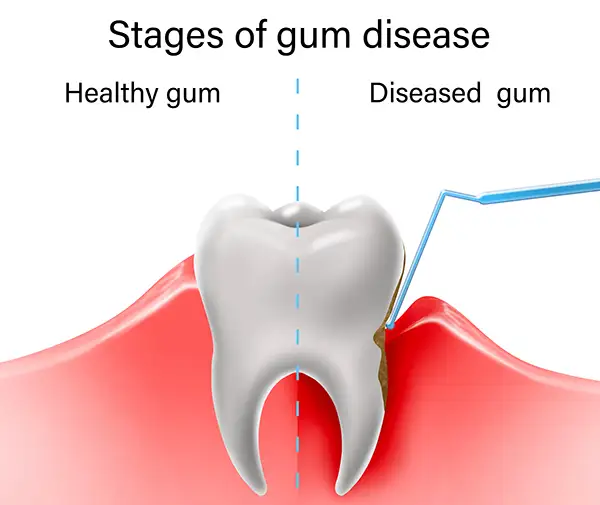
The connection between diabetes and gum disease is well-established and bidirectional. Higher blood sugar means more glucose in your saliva and gum tissue, which feeds the bacteria that cause gum infections. At the same time, diabetes blunts your immune system’s ability to clear those infections. Going the other direction, treating active gum inflammation has been shown in clinical research to modestly improve glycemic control. The two systems talk to each other.
What Changes About Your Dental Visits
For diabetic patients who develop gum disease, the biggest practical change is recall frequency. Six-month cleanings aren’t enough; we recommend periodontal maintenance every three months instead, so we’re ahead of the inflammation rather than chasing it. We also schedule appointments around your insulin and meals when it matters – if you take morning insulin and you’re going to be sitting through a longer procedure, late morning or early afternoon is usually safer than first thing in the morning while you’re still fasting. When your case is more involved, we coordinate with your primary care provider or endocrinologist before larger procedures.
Risks Worth Watching For
Beyond gum disease, you may notice dry mouth more often, sometimes from medications and sometimes from the diabetes itself. Dry mouth isn’t just uncomfortable – saliva is one of your main defenses against decay, so reduced flow accelerates cavities. Other things we watch for: oral thrush (a fungal infection more common when blood sugar runs high), changes in taste, and slower healing after extractions and similar procedures. None of these are guaranteed, and well-controlled diabetes substantially lowers the risk on each.
Dental Implants and Diabetes
A common question we hear is whether dental implants are still on the table for diabetic patients. The honest answer is usually yes, with a caveat. Well-controlled diabetes is not a contraindication for implants, and outcomes for these patients track close to non-diabetic patients in most clinical studies. Poorly controlled diabetes raises implant failure risk, mostly because of impaired healing and higher infection risk during the months when the implant is fusing to bone. We talk through your A1C trajectory with you – never as a replacement for what your medical team is doing, but to set realistic expectations about timing.
Your Diabetic Dental Care Team in Scottsdale
Dr. Rod W. Gore has been practicing dentistry in Scottsdale for over 38 years. He earned his Doctor of Dental Surgery from Northwestern University in 1987 and is one of only two dentists in Arizona who hold AACD Accredited Member status. The credential is best known for cosmetic work, but the same case-planning discipline – documenting baseline tissue conditions, sequencing treatment, watching how gums respond visit to visit – carries directly into managing the oral health of patients with chronic conditions like diabetes. Full background on Dr. Gore’s bio page.
Dr. Brynn Van Dyke, DMD, completed her dental training at Midwestern University in Glendale, Arizona, after spending nearly five years as a dental assistant before dental school. That chairside time matters here. Working well with diabetic patients often comes down to small adjustments – how you schedule, what you watch for, how you adjust the cleaning depending on tissue response – that come from years of hands-on experience. More on her bio page.
What Your Visit Looks Like as a Diabetic Patient
 Four parts of the visit work differently for a diabetic patient: front-desk check-in, the cleaning itself, what we ask of you afterward, and how often you come back. None is dramatic on its own. Together, they account for diabetes without making the visit more complicated than it needs to be. Four parts of the visit work differently for a diabetic patient: front-desk check-in, the cleaning itself, what we ask of you afterward, and how often you come back. None is dramatic on its own. Together, they account for diabetes without making the visit more complicated than it needs to be.
Pre-Visit Check-In
At the front desk we ask about your most recent A1C if you know it, what diabetes medications you’re on, when you last took insulin or oral medications, and when you last ate. We don’t share any of it without your permission – we ask because all of it changes how we plan the appointment. If you don’t know your most recent A1C, that’s fine; we work with what you have.
The Cleaning Itself
For patients with active gum inflammation, we look at probing depths in more detail than a standard cleaning, and we may recommend localized antimicrobial therapy along with the standard scaling. If your gums bleed easily during the cleaning, that’s information we use to guide the next steps – not a reason to put off coming back. We adjust the cleaning to avoid creating more bleeding than necessary while still removing the bacterial load that’s driving the inflammation.
Post-Visit Considerations
After certain procedures – extractions, deeper periodontal work, anything that breaks the gum tissue – we send you home with specific instructions on managing your blood sugar and oral hygiene during healing. Diabetic patients heal more slowly on average, and gentle, on-schedule home care matters more than usual during the first week. If a procedure is involved enough to warrant pre-medication or coordination with your physician, we handle that ahead of time.
Recall and Follow-Up
Patients whose diabetes is well-controlled and who don’t have gum disease typically stay on a six-month schedule with closer attention at each visit. For patients with active or historical gum disease, we shift to three-month periodontal maintenance instead. We work out the right cadence with you rather than defaulting to a number on a chart.
Benefits of Diabetes-Aware Dental Care
The most direct benefit of consistent, diabetes-aware dental care is fewer surprises. Gum disease that gets caught at the gingivitis stage is reversible; gum disease that’s been progressing quietly for two years often isn’t. Closer-spaced visits give us more chances to catch the early signs before they progress past the reversible stage.
There’s also a feedback loop that often surprises patients. Many people who address chronic gum inflammation see their fasting glucose and A1C edge in the right direction over the following months. The change isn’t dramatic, and it’s not a substitute for medical care, but the cooperation between dental health and overall health is real and worth taking advantage of.
A practical benefit that’s easy to overlook: dry mouth, fungal flare-ups, and the small dental issues that come along with diabetes are much easier to handle when you have an established relationship with a dental team that knows your history. Calling us about a sore patch or a sudden taste change is faster than starting from scratch with someone new.
Why Choose Our Practice for Diabetic Dental Care
The most useful filter for choosing a dentist for diabetic care is whether the practice will actually slow down with you. Not every office adjusts visit length, recall frequency, and treatment sequencing for chronic medical conditions. We do, because the alternative is rushing through cleanings that miss what matters in patients whose mouths are responding to a moving target.
Continuity of staff helps too. Shawna, our hygienist, has been with our practice since 2007, so when she sees a change in your tissue response she knows whether that’s normal for you or something new. That continuity is the difference between catching a flare-up at the next visit and finding it three appointments later when it’s harder to reverse.
What our patients say about working with us:
"I have been a patient of Dr. Gore since 1995 when I moved to the valley. He and his entire staff have take such great care of my family and I over the years. My wife who became significantly disabled in the past few years requires extra care now and Dr. Gore and his team have been amazing with her. They provide superb dental care to her, but more so, they are very compassionate and very understanding of her special needs."
– Ed C., Google review
"I have been a patient of Dr Gore’s for a decade and what a difference a great dentist makes! My gums were in very bad condition but he set up a recovery plan to get them healthy. Shawna is by far the best dental hygienist I’ve ever been to and I wouldn’t let anyone else near me for my cleanings absolutely amazing with the best bedside manner ever."
– Tiffany C., Google review
"My elderly mother has dementia and I was told by the staff at her senior living center that she had been spitting blood and was having trouble eating. I brought her to Dr. Gore and she needed several root canals due to her neglecting her teeth. He made sure she was comfortable and couldn’t have been nicer."
– Robin M., Google review
Cost and Insurance for Diabetic Dental Care
Cost is a fair concern, especially when the recommended schedule is three-month visits instead of six-month. Here’s the honest part: most dental insurance plans pay for two cleanings per year as preventive, then cover periodontal maintenance visits at a different rate after a documented gum disease diagnosis. The benefit you actually get depends on your specific plan, your annual maximum, and how the periodontal coding has been recorded in your chart. We accept Cigna and Guardian PPO and most other major PPO plans, and our front office team verifies your benefits and submits out-of-network claims when they apply. Our financial and insurance page has the carrier list and walks through how we handle claims.
For patients without dental insurance, our in-office GOREgeous Membership Plan covers two exams and two cleanings a year, X-rays, and discounts on additional treatment for a flat annual fee. For diabetic patients on a three-month maintenance schedule, the math usually works out in your favor compared with paying out-of-pocket per visit. We can walk through the numbers with you at your consultation so you know what your year of dental care will actually cost.
Schedule Your Visit
If you have diabetes and it’s been a while since your last cleaning, come in. Call GOREgeous Smiles at 480-585-6225 or use our Request an Appointment page to schedule. We’re at 8535 E. Hartford Drive #208 in Scottsdale, AZ 85255-5438. You can get directions on Google Maps or reach our team through our Contact page with any questions before booking.
Frequently Asked Questions
Do I really need to come in every three months instead of every six?
Many diabetic patients do, especially those with active gum disease, but six-month cleanings still work fine for patients without periodontal involvement and with stable A1C. For patients with documented gum disease – bleeding pockets, attachment loss, ongoing inflammation – three months is the gap before bacterial regrowth typically reaches a level that drives more damage. We make the call together based on what we see, not on a rule applied to every diabetic patient.
Should I tell you my A1C number when I come in?
It’s helpful but not required. A recent A1C tells us how well your blood sugar has been controlled over the past few months, which affects how we plan around healing for any procedure beyond a basic cleaning. If you don’t know yours, we can still do everything; the number just helps us calibrate. We don’t share it with anyone outside the practice without your written authorization.
Are dental implants safe for me with diabetes?
Often, yes. The most important factor isn’t whether you have diabetes – it’s whether your blood sugar has been under reasonable control in the months around the procedure. Most implant studies don’t show significantly different long-term success rates between non-diabetic patients and diabetic patients whose A1C values are within the range their physician considers stable. If your control has been a moving target recently, we may suggest waiting until things settle before placing the implant rather than canceling the option altogether.
Will treating my gum disease lower my blood sugar?
Modestly, in many cases. The clinical research on this points to small but real reductions in A1C – often in the range of 0.3 to 0.5 percentage points – following successful periodontal treatment in patients with both gum disease and Type 2 diabetes. That’s not a substitute for what your physician is doing with diet, medication, or insulin. It’s an additional contribution from a different direction.
What time of day should I schedule my appointment?
For most diabetic patients in Scottsdale, late morning or early afternoon works best, especially for longer procedures. Right after breakfast and a normal medication routine, blood sugar tends to be more stable than first thing in the morning while you’re still fasting. If you take long-acting insulin or have unusual scheduling needs, just tell our front office and we’ll work around your routine.
What if my diabetes isn’t well-controlled right now?
Come in anyway. Routine cleanings and exams are not where blood sugar control becomes a barrier; we adapt those to your situation regardless. We may recommend deferring elective procedures – cosmetic work, implants, large restorations – until your numbers settle into a more predictable range. The dental side of catching cavities and managing gum inflammation matters even more during a period when your control is shifting, not less.
If I need cleanings every three months, how do most insurance plans handle that?
The coding shifts more than the coverage. Once gum disease is on your chart, third and fourth visits in a year are typically billed as periodontal maintenance rather than routine cleaning, which falls under a different benefit category in most PPO plans. Some plans cover four maintenance visits annually; others cap at two. Your annual maximum is usually the bigger constraint than the per-visit code. Our front office runs those numbers before treatment so you know what your year looks like before you commit. |
 If you have diabetes, the standard recall schedule isn’t always the right fit, and at GOREgeous Smiles in Scottsdale, AZ, we adjust your visits to match how diabetes actually affects your mouth. Chronically elevated blood sugar feeds inflammation in gum tissues and slows the body’s response to bacterial infection, which is why gum disease tends to be more common, more aggressive, and harder to control in patients with diabetes than in the general population.
If you have diabetes, the standard recall schedule isn’t always the right fit, and at GOREgeous Smiles in Scottsdale, AZ, we adjust your visits to match how diabetes actually affects your mouth. Chronically elevated blood sugar feeds inflammation in gum tissues and slows the body’s response to bacterial infection, which is why gum disease tends to be more common, more aggressive, and harder to control in patients with diabetes than in the general population. Dental care for diabetic patients is the same dentistry – cleanings, exams, fillings, restorations – adjusted for how diabetes changes the mouth. The differences aren’t dramatic on most days, but they add up over time, and small adjustments now prevent a lot of problems we’d otherwise have to treat later.
Dental care for diabetic patients is the same dentistry – cleanings, exams, fillings, restorations – adjusted for how diabetes changes the mouth. The differences aren’t dramatic on most days, but they add up over time, and small adjustments now prevent a lot of problems we’d otherwise have to treat later. Four parts of the visit work differently for a diabetic patient: front-desk check-in, the cleaning itself, what we ask of you afterward, and how often you come back. None is dramatic on its own. Together, they account for diabetes without making the visit more complicated than it needs to be.
Four parts of the visit work differently for a diabetic patient: front-desk check-in, the cleaning itself, what we ask of you afterward, and how often you come back. None is dramatic on its own. Together, they account for diabetes without making the visit more complicated than it needs to be.