Sleep Apnea Treatment in Scottsdale, AZ
If CPAP isn’t working for you, GOREgeous Smiles designs custom oral appliances for sleep apnea and snoring at our office in Scottsdale, AZ. Dr. Rod W. Gore has been fabricating these appliances chairside for years, and the videos above show what the switch from CPAP to a dental appliance looks like for patients who couldn’t tolerate the mask.
Sleep apnea is more than a sleep problem. When breathing repeatedly stops during the night, oxygen drops and the heart works harder. Published research links untreated obstructive sleep apnea to cardiovascular disease, hypertension, GERD, and reduced life expectancy. The encouraging news is that for people with mild-to-moderate OSA, or for anyone who has tried CPAP and given up on it, a custom-made oral appliance is a recognized alternative therapy that works alongside your sleep physician’s care.
We don’t diagnose sleep apnea here. A sleep physician handles the diagnosis, often through an overnight in-lab study or a home sleep test. Once you have a diagnosis and a recommendation for oral appliance therapy, we take it from there: scans, fabrication of the appliance in our own office using 3D-printing dental technology, fitting, follow-up, and adjustment over time. If you’ve already had a sleep study and your doctor has cleared you for an oral appliance, we can move quickly. If you’re earlier in the process, we’ll help you figure out the next step.
On This Page
What Is Sleep Apnea?
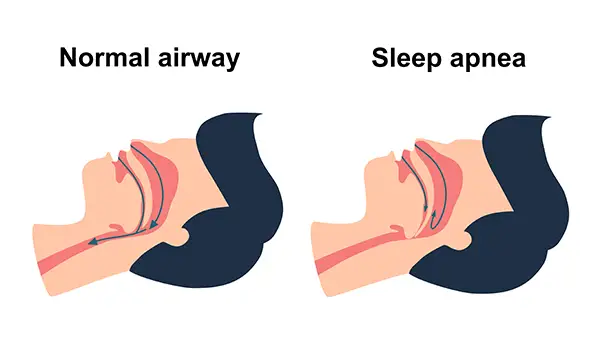 Sleep apnea is a condition where breathing stops and starts repeatedly during sleep. The most common form, obstructive sleep apnea (OSA), happens when the soft tissues at the back of the throat collapse against the airway, blocking airflow until the brain partially wakes you to take a breath. This can happen dozens or hundreds of times per night without you remembering any of it. Sleep apnea is a condition where breathing stops and starts repeatedly during sleep. The most common form, obstructive sleep apnea (OSA), happens when the soft tissues at the back of the throat collapse against the airway, blocking airflow until the brain partially wakes you to take a breath. This can happen dozens or hundreds of times per night without you remembering any of it.
Sleep apnea is not the same thing as snoring, although the two often travel together. The American Academy of Sleep Medicine recognizes oral appliance therapy as an evidence-based treatment for mild-to-moderate OSA, and as an option for severe OSA in patients who can’t tolerate CPAP.
Snoring vs. Sleep Apnea
Snoring is the noise. Apnea is the breathing pause. Loud, regular snoring is one of the strongest patient-reported signals that obstructive sleep apnea may be present, but plenty of people snore without apnea, and some apnea patients don’t snore loudly. The way to tell them apart is a sleep study. We see patients in both groups: people who came in because their partner couldn’t sleep next to the snoring, and people who came in already diagnosed and looking for a CPAP alternative.
Obstructive Sleep Apnea (OSA)
OSA is the form of sleep apnea most commonly treated with a dental device. Risk factors include enlarged tonsils, narrow upper airway anatomy, neck circumference, body weight, and family history. The standard diagnostic path is a sleep study ordered by a sleep physician, typically scored using the apnea-hypopnea index (AHI). Patients with mild-to-moderate AHI scores are the most likely to do well on oral appliance therapy. For severe OSA, sleep physicians usually prescribe CPAP first. An oral appliance comes in as the alternative when patients can’t tolerate CPAP.
Oral Appliance Therapy
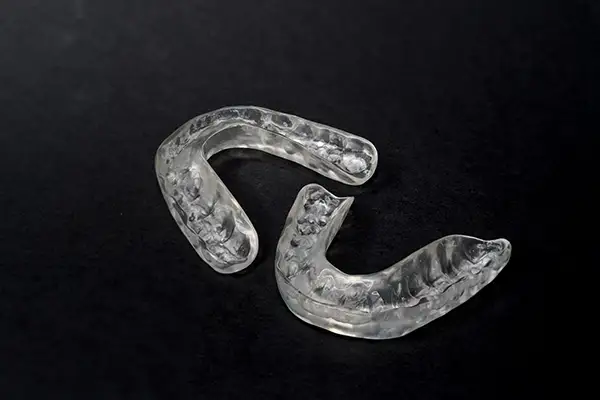
Oral appliance therapy uses a custom-fabricated dental device, also called a mandibular advancement device or MAD, that you wear while you sleep. The appliance gently holds the lower jaw forward, which keeps the tongue base from collapsing against the back of the throat. The result is an open airway and uninterrupted breathing through the night.
The appliance we make is custom for your mouth. We take impressions or digital scans, design the device for your bite, and fabricate it in-house using our 3D printing technology. That means quicker turnaround, easier adjustment if something doesn’t sit right, and a fit you can’t get from an over-the-counter product. The boil-and-bite mouthpieces sold online are not the same thing – they aren’t sized to your bite, they don’t track jaw position, and the wrong fit over months can shift teeth or strain the joint.
Most patients describe the first week or two as an adjustment period. Some dryness in the mouth, mild jaw soreness, and light tooth sensitivity are common and usually settle within the first few weeks. We see you back for an adjustment visit so the device sits the way it should.
When CPAP Isn’t Working
The biggest reason patients arrive at our office for an oral appliance is that they tried CPAP and couldn’t tolerate it. Mask claustrophobia, noise, dry sinuses, the inability to sleep on your side, the hassle of travel – the device is clinically effective, but adherence is the hard part. If you’ve been prescribed CPAP and given up on it, you’re not failing treatment; you’re describing the most common reason oral appliance therapy exists. We coordinate with your sleep physician to confirm that an appliance is the right next step for your case.
TMJ and Bruxism Overlap
Many of the patients we see for sleep apnea also clench or grind their teeth at night, and a smaller subset have ongoing jaw joint pain. The connection isn’t always direct, but disrupted sleep and airway compromise can drive nighttime muscle activity. If you’re being evaluated for sleep apnea and also have jaw pain, headaches, or worn enamel, we may discuss TMJ treatment and custom mouth guards alongside the sleep appliance, and in some cases therapeutic Botox for jaw and headache pain when muscle hyperactivity is the bigger driver. Each of these is a separate conversation; the point is that the conditions overlap and we’ll address them together if relevant.
Your Sleep Apnea Care Team in Scottsdale
Dr. Rod W. Gore has been practicing dentistry in Scottsdale for more than 38 years, and he’s been fabricating oral appliances for sleep apnea patients in this office for years. The clinical work for these cases – impressions, design, in-office milling and 3D printing, fitting, follow-up adjustment – is what he does day in and day out. Full background on Dr. Gore’s bio page.
Dr. Gore is also one of only two dentists in Arizona who hold AACD Accredited Member status. AACD Accreditation is for cosmetic case work rather than sleep medicine specifically, but the skill set translates. The same hands that fit a porcelain restoration to a fraction of a millimeter are the hands fitting an oral appliance to your bite.
The other half of the team is Dr. Brynn Van Dyke, DMD, who completed her Doctor of Dental Medicine at Midwestern University in Glendale. Before dental school she spent close to five years working as a dental assistant, which gave her an unusual amount of chairside experience before she ever started practicing. She works with patients across our full range of services, including those who come in for sleep apnea care. More on her bio page.
We are not board-certified sleep physicians, and we do not diagnose sleep apnea. A sleep physician makes the diagnosis based on a sleep study. What we do is the dental side: working from your sleep doctor’s recommendation to fabricate, fit, and adjust the oral appliance.
The Sleep Apnea Care Process
 Patients come to us at different points in the process. Some have just had a sleep study and are looking for an alternative to CPAP. Some haven’t been tested yet and want to know whether they should be. The four stages below describe what happens once you’re seeing us specifically for the appliance. Patients come to us at different points in the process. Some have just had a sleep study and are looking for an alternative to CPAP. Some haven’t been tested yet and want to know whether they should be. The four stages below describe what happens once you’re seeing us specifically for the appliance.
1. Initial Conversation and Screening
We start with what brought you in. Are you snoring? Has your partner noticed you stopping breathing at night? Are you tired during the day even after a full night of sleep? Have you already been tested? Have you tried CPAP? Sleep apnea warning signs often surface first during a routine dental cleaning, when a hygienist notices tooth wear from grinding or other clinical signals. We’ll also do a basic look at the airway anatomy and tonsil size, and check for tooth wear that suggests nighttime grinding. If you haven’t been formally diagnosed and there are clinical signs pointing to sleep apnea, the next step is a sleep study, not an appliance.
2. Diagnosis and Coordination With Your Sleep Physician
A sleep apnea diagnosis comes from a sleep study, either in a sleep lab overnight or via a home sleep test you do in your own bed. We coordinate with sleep physicians in the Scottsdale area to make this referral straightforward, and many of our patients qualify for a home sleep test. That’s how most of the patients on the videos above did it. Once your sleep physician confirms the diagnosis and recommends oral appliance therapy, we have what we need to proceed.
3. Appliance Fabrication and Fitting
With the diagnosis in place, we take precise impressions or digital scans of your upper and lower teeth and design the appliance for your bite. We fabricate the device in-house using our 3D printing technology, which gives us tight control over the fit and a faster turnaround than sending the case to an outside lab. At the fitting visit, we check the position of the lower jaw, the comfort of the appliance against your teeth and gums, and the way it tracks when you open and close. You’ll wear it that night.
4. Follow-Up and Long-Term Adjustment
We see you back a few weeks after the fitting to check how the appliance is wearing, how your sleep has changed, and whether to advance the lower jaw position further. Most appliances are adjustable in small increments, and we refine the ideal jaw position over the first month or two. Beyond that, regular dental exams are the right place to keep an eye on tooth wear, jaw joint function, and the appliance itself. If signs of bruxism develop or worsen, we’ll talk about whether a separate guard for daytime use, or a different appliance design, would help.
Benefits of Oral Appliance Therapy
The most immediate benefit patients describe is sleep itself. When the airway stays open through the night, the brain doesn’t have to keep waking you every few minutes to restart breathing, and morning energy improves quickly. Patients who have spent months or years in chronic exhaustion often notice the difference within a week of consistent appliance use. The second video on this page shows what that change looks like in someone’s daily life.
Snoring usually decreases substantially because the airway position that causes the noise is the same airway position the appliance corrects. For couples where snoring has been a long-running source of disrupted sleep on both sides of the bed, that change has its own value separate from the medical reasons for treatment.
The cardiovascular and metabolic load of untreated sleep apnea is well documented. Repeatedly dropping oxygen levels during sleep stresses the heart, and untreated OSA correlates with hypertension, atrial fibrillation, and reduced life expectancy. We don’t promise that wearing an appliance reverses these risks, but we can say that for patients who reach effective treatment, the appliance addresses the underlying mechanism that drives the risk.
Compared with CPAP, the practical benefits of an oral appliance are mostly about adherence. There’s no mask, no electricity required, no tubing to manage, and the device fits in a small case for travel. CPAP is generally more effective per-night for severe OSA, which is why patients with severe OSA usually start on CPAP. For patients who use a CPAP and benefit from it, we don’t try to talk them off it. For patients who can’t, the appliance is often what makes treatment possible.
Why Choose Our Practice for Sleep Apnea Care
The most important factor when choosing a dental office for an oral appliance is whether the doctor actually fabricates these regularly. A device that doesn’t fit well, isn’t titrated correctly, or sits poorly against the teeth is worse than no device at all. Dr. Gore has been making oral appliances for sleep apnea patients in this office for years, and we design and build the appliances here using our SprintRay 3D printing technology. Outside dental labs are fine, but in-house fabrication shortens the timeline, makes adjustments faster when something needs to change, and keeps the dentist who designed the appliance in direct contact with how it sits in your mouth.
We work in coordination with sleep physicians rather than around them. If a sleep physician you trust has already diagnosed you, we use their report to drive the appliance design. If you haven’t had testing yet, we’ll help you get into the right testing pathway, including arranging a home sleep test where appropriate. The model is that the sleep physician handles diagnosis and ongoing medical management, and we handle the dental device.
Senior dental care is a big part of what we do, and sleep apnea prevalence rises with age. Patients in their 50s through 70s come to us in two groups: people who have tolerated CPAP for years and now want a switch, and people who were recently diagnosed and want to start with an appliance. We see these cases regularly. More patient feedback on our reviews page.
Cost and Insurance for Sleep Apnea Treatment
Cost depends on the case, and the insurance situation for sleep apnea treatment is different from most dental work. Insurance carriers usually process oral appliance therapy under medical coverage rather than dental, because the underlying diagnosis is a medical condition, not a dental one. Coverage varies considerably by plan. Some plans cover most of the appliance after your deductible, some cover a portion, and some don’t apply at all. Our front office team verifies both your medical and dental benefits before fabrication, so you know what your plan pays for and what you’ll pay out of pocket.
If your coverage doesn’t apply, the GOREgeous Membership Plan includes a sleep apnea consultation as one of its benefits and provides a discount on additional treatment. For patients who would rather spread the cost over time, we offer third-party financing options so an appliance can fit a monthly budget rather than landing all at once. Our financial and insurance page lists accepted plans and outlines how we handle the medical-versus-dental insurance distinction. Call 480-585-6225 for a personalized estimate.
Schedule a Sleep Apnea Consultation in Scottsdale
If snoring or sleep apnea is keeping you or your partner from real rest, the first step is a conversation. Call GOREgeous Smiles at 480-585-6225 or use our Request an Appointment page to schedule. We’re located at 8535 E. Hartford Drive #208 in Scottsdale, AZ 85255-5438. You can also reach us through our Contact page with any questions before booking.
Frequently Asked Questions
Can a dentist diagnose sleep apnea?
No. A formal diagnosis of sleep apnea comes from a sleep physician based on a sleep study, either an in-lab study or a home sleep test. Dentists are often the first providers to spot the warning signs – tooth wear from grinding, airway anatomy, the partner-reported snoring history – and we coordinate the referral, but the diagnosis itself is medical. Once your sleep doctor confirms the diagnosis and recommends oral appliance therapy, we handle the dental side from there.
What is the difference between a custom oral appliance and the ones sold online?
We fabricate a custom appliance from impressions or scans of your specific bite. It accounts for jaw position, tooth alignment, and the amount of mandibular advancement that’s right for your case, and it’s adjustable. Over-the-counter boil-and-bite devices are one-size-with-some-flexibility, and they don’t track or correct jaw position. Wearing the wrong device for months can shift teeth or strain the jaw joint. A common reason patients come in for a custom appliance is having tried an online one and run into fit or jaw issues.
Will an oral appliance change my bite over time?
Small bite changes are possible with long-term oral appliance therapy, which is part of why follow-up matters. The trade-off is usually clinically minor compared with the consequences of untreated sleep apnea. We monitor bite, jaw joint function, and tooth wear at follow-up visits and adjust the appliance design or recommend additional steps if anything needs attention. Patients who keep up with their dental visits catch any changes early.
Is oral appliance therapy covered by insurance?
Most carriers process oral appliances for sleep apnea through medical insurance, not dental, because the underlying diagnosis is medical. The two most useful questions to ask your medical insurance carrier before fabrication are whether they cover code E0486 (the standard HCPCS code for a custom oral appliance for OSA) and whether you have a current sleep study on file. Our front office makes those calls for you and walks you through what’s covered before we move ahead.
Does an oral appliance work as well as CPAP?
For mild-to-moderate obstructive sleep apnea, the published evidence shows oral appliance therapy and CPAP often produce similar real-world outcomes, with the appliance typically having higher patient adherence because it’s easier to live with. For severe OSA, CPAP is generally more effective on a per-night basis, but the gap closes when you account for how often patients actually wear each device. The most effective treatment is usually the one a patient will actually use every night.
How long until I notice a difference?
Most patients describe an improvement in morning energy and partner-reported snoring within the first week or two of consistent use. The first few nights are often a mixed adjustment – the appliance feels new in your mouth, your jaw position is different – but the sleep benefit shows up quickly once the device is comfortable. Optimal jaw position usually takes a couple of follow-up adjustments to dial in over the first month.
What are the common side effects?
The most common are dry mouth in the morning, mild jaw soreness for the first few weeks, and occasional tooth sensitivity. Most of these settle within the adjustment period. Less common but worth knowing about: small bite changes over time and occasional jaw joint discomfort, both of which we monitor at follow-up. We evaluate patients with active TMJ pain case by case to decide whether an oral appliance, a different design, or a different approach altogether is the right call.
Why choose this practice for sleep apnea care in Scottsdale?
The two most important questions to ask any dentist offering oral appliance therapy are how often they fabricate these appliances and where the device is made. We make ours in this office using SprintRay 3D printing, which gives us same-week turnaround on most cases and direct control over fit and titration. Dr. Gore has been doing this work in Scottsdale for years, and we coordinate with sleep physicians rather than diagnosing in isolation. If those things matter to you, we’re a good fit.
|
 Sleep apnea is a condition where breathing stops and starts repeatedly during sleep. The most common form, obstructive sleep apnea (OSA), happens when the soft tissues at the back of the throat collapse against the airway, blocking airflow until the brain partially wakes you to take a breath. This can happen dozens or hundreds of times per night without you remembering any of it.
Sleep apnea is a condition where breathing stops and starts repeatedly during sleep. The most common form, obstructive sleep apnea (OSA), happens when the soft tissues at the back of the throat collapse against the airway, blocking airflow until the brain partially wakes you to take a breath. This can happen dozens or hundreds of times per night without you remembering any of it. Patients come to us at different points in the process. Some have just had a sleep study and are looking for an alternative to CPAP. Some haven’t been tested yet and want to know whether they should be. The four stages below describe what happens once you’re seeing us specifically for the appliance.
Patients come to us at different points in the process. Some have just had a sleep study and are looking for an alternative to CPAP. Some haven’t been tested yet and want to know whether they should be. The four stages below describe what happens once you’re seeing us specifically for the appliance.